| Table of Contents |  |
|
Case Report
|
| Spontaneous subclavian vein thrombosis — a source of pulmonary embolism in young man manifested by pleural effusion: A case report |
| Margita Belicová1, Hubert Poláček2 |
|
1Department of Internal Clinic University Hospital, Kolarova 2, 036 59 Martin, Slovakia.
2Department of Radiologic Clinic University Hospital, Kollarova 2, 036 59 Martin, Slovakia. |
|
doi:10.5348/ijcri-2012-06-139-CR-12
|
|
Address correspondence to: Margita Belicová Department of Internal Clinic University Hospital Kolarova 2 036 59 Martin Slovakia Email: mbelicova@hotmail.com |
|
[HTML Abstract]
[PDF Full Text]
|
| How to cite this article: |
| Belicová M, Poláček H. Spontaneous subclavian vein thrombosis — a source of pulmonary embolism in young man manifested by pleural effusion: A case report. International Journal of Case Reports and Images 2012;3(6):50–53. |
|
Abstract
|
|
Introduction:
Spontaneous upper-extremity deep venous thrombosis is associated with exercise, occurs in young healthy individuals and can be source of pulmonary embolism.
Case Report: This case illustrates a 26-year-old Caucasian, left-handed, healthy man with overlooked subclavian vein thrombosis, which was source of pulmonary embolism. Pulmonary embolism manifested with pleural effusion and at the beginning was treated as tuberculous pleuritis. Conclusion: In this case, pulmonary embolism manifested with repeating chest pain due to pleural effusion. Source of embolus was an overlooked left subclavian vein thrombosis. Underlying anatomical abnormalities in this case was adherent first and second ribs, causing compression of the subclavian vein. Incorrect diagnosis at the beginning was the cause of delayed treatment. | |
|
Key Words:
Upper-extremity deep venous thrombosis, Paget-von schroetter syndrome, Pulmonary embolism
| |
|
Introduction
| ||||||
|
Sir James Paget first described thrombosis of the subclavian veins in 1875 [1] and in 1884, von Schrötter postulated that this syndrome resulted from occlusive thrombosis of the subclavian and axillary veins. [2] In recognition of the work of these pioneers, in 1949, Hughes coined the term Paget-von Schrötter syndrome. [3] It usually results from the excessive use of the involved arm by predisposed individuals. Upper-extremity deep vein thrombosis (UEDVT) is an increasingly important clinical entity with potential for considerable morbidity. Complications include post-phlebitic limb syndrome from resultant valvular incompetence, venous gangrene and pulmonary embolism (PE). PE is present in up to one third of patients with UEDVT. [4] | ||||||
|
Case Report
| ||||||
|
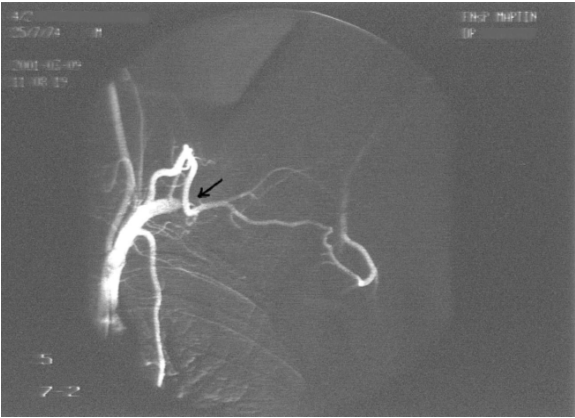
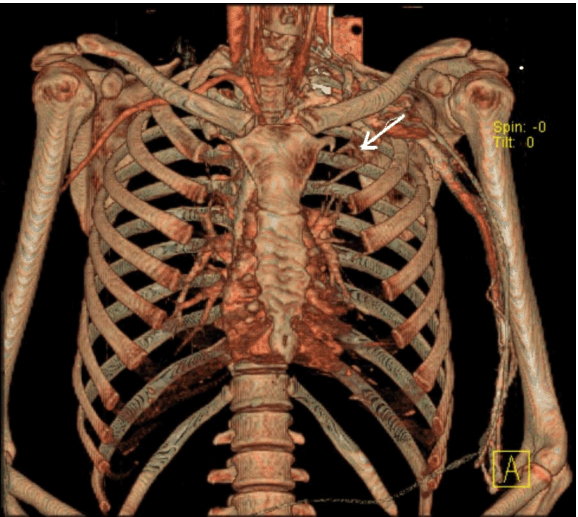
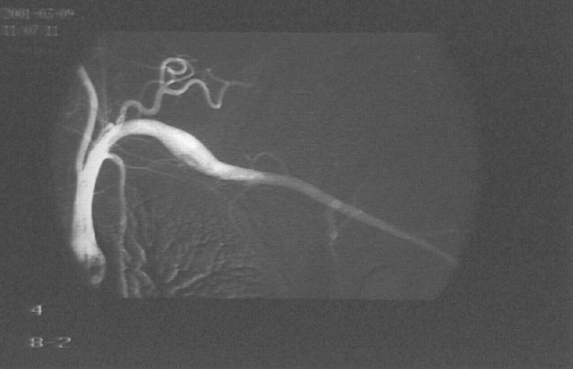
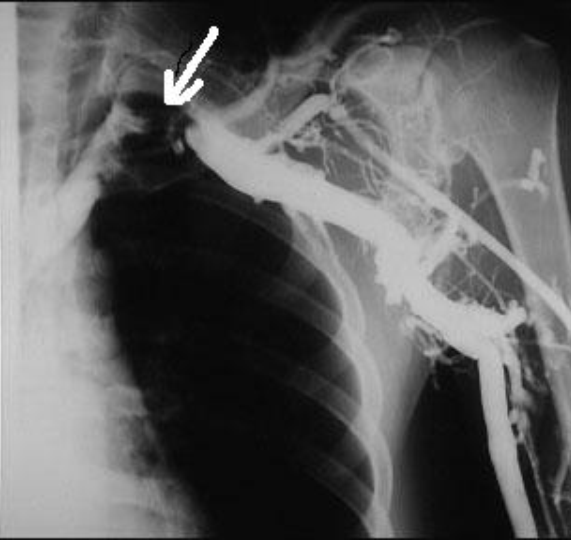
A 26-year-old left-handed healthy man presented with a three month history of repeated bilateral chest pain. Six months previously, he started heavy muscular activity of upper limbs (work out at a gym). Two months before he had been examined by his pulmonologist because chest X-ray revealed bilateral small effusion and tuberculin test had been positive. The patient started treatment as suspected tuberculous pleuritis and beside antituberculous drugs he used corticoids too. Despite treatment, difficulties remained and the patient was remitted to our clinic. On examination, there was no edema of the left arm, only prominent superficial veins on arm and left part of chest. On auscultation of the lungs, breath sounds were weakened bilaterally. Chest radiography revealed small pleural effusion. Electrocardiography and echocardiography were normal. Suspected pulmonary embolism was confirmed by computed tomography. DVT in lower limb was excluded by compression ultrasonography. Because the patient had prominent superficial veins on arm and left part of chest, we suspected left subclavian vein thrombosis, which was established by venography (Figure 1). Aortography revealed aneurysm of left subclavian artery (Figure 2) and also confirmed left thoracic outlet syndrome due to adherent first and second ribs (Figure 3), interruption of flow in left subclavian artery in abduction of left upper limb and appropriate flow in left subclavian artery in adduction of left upper limb (Figure 4). Patient was administered low molecular weight heparin as initial step, followed by the acenocoumarol therapy. A thrombophilia screen revealed prothrombin 20210A mutation, which was detected by polymerase chain reaction. Adequate medical anticoagulant treatment with low molecular weight heparin followed by coumarin led to significant clinical upturn and coumarin was stopped after six months. After six months the patient presented to the vascular surgeon, who performed resection of adherent first and second ribs (Figure 5). For two weeks after surgery, the patient was administerd low molecular weight heparin followed by aspirin. Nowadays, nine years after surgery, the patient has experienced complete resolution of his symptoms, his prominent superficial veins on arm and left part of chest have disappeared and he has used no medication. The CT-angiography confirmed complete resolution DVT of left subclavian vein (Figure 6). | ||||||
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
|
Discussion
| ||||||
|
Spontaneous subclavian or axillary vein thrombosis comprises 2% of all depp vein thrombosis (DVT). The mean age is 30 years, both genders are affected equally and there is a predilection for the dominant arm. Patients with subclavian vein thrombosis may describe a history of trauma or more frequently, strenuous use of the arm (>50% cases). Common precipitating activities involve repeated hyperabduction and external rotation of the arm or backward and downward rotation of the shoulder. [5] The mechanism for subclavian vein thrombosis is thought to be extrinsic compression of the subclavian vein within a tunnel comprising the first rib inferiorly, the subclavius muscle superiorly, the costoclavicular ligament medially and the anterior scalene muscle laterally. Abnormalities such as a laterally inserting costoclavicular ligament or cervical rib (10%) can compress the subclavian vein, predisposing to thrombosis. This is termed "effort thrombosis" or "thoracic outlet obstruction syndrome". [6] In this case, there was a clear precipitant, gymnastics maneuvers for last six month and there was the adherent first and second ribs as cause of exstrinsic compression of subclavian vein. Annual incidence of upper thoracic outlet syndrome ranges between 3–80 new cases for 1000 individuals, and it typically affects younger individuals aged between 20 and 50 years. [7] Not all patients with subclavian vein thrombosis are symptomatic. Those with symptoms may present with mild-to-moderate non-pitting edema and mild cyanosis of the hands and fingers on the affected side. Dilatation of subcutaneous collateral veins may be present over the upper arm and chest. This later sign may be the only clue to UEDVT in otherwise asymptomatic patiens. In a few cases, in which the diagnosis was missed or delayed or the patient presented late, the thrombus may have extended to the superior vena cava or be the cause of PE. In addition, patients with UEDVT less often have clinically overt PE than those with lower-extremity DVT. [8] PE is a common and a potentially life threatening condition associated with considerable morbidity and mortality. Pleural effusions are a common occurrence in patients with PE, which is also a disorder commonly overlooked in the work-up of a patient with pleural effusion. [9] In this case, the patient presented with no edema on afected side, had only dilatation of subcutaneous collateral veins over the left upper arm and chest and diagnosis of UEDVT was overlooked. PE manifested with pleural effusion and diagnosis was overlooked too. Patient was administered antituberculous drugs and corticoids because of incorrect diagnosis of tuberculous pleuritis at the beginning. Incorrect diagnosis was made, because patient had positive tuberculin skin test, which can be false positive. [10] Prompt diagnosis of UEDVT allows right treatment and impoves the clinical outcome. The presence of thrombus may be established by duplex ultrasonography examination, venography, magnetic resonance angiography or computerized tomography (CT). Colour duplex ultrasonography is the best initial evaluation because it is non-invasive and has a high sensitivity and specificity. In turn, venography is still the 'gold standard' in evaluating subclavian and axillary vein thrombosis. Upper extremity venography is a cost effective imaging examination, and a normal image for upper extremity venography should reveal bilateral, symmetric, rapid, and smooth radiolabeled radiotracer flow from the upper extremities to the central venous systém. [11] In this case, venography revealed left subclavian vein thrombosis, thoracic radiography showed left adherent first and second ribs. The initial measures commonly used are based on rest and elevations of the affected limb followed by anticoagulation. Both conservative and surgical therapy (anticoagulation, systemic or catheter directed thrombolytic therapy, thrombectomy, balloon angioplasty followed by stenting) are common alternative treatments for UEDVT. From the physician's standpoint, the optimal management of subclavian vein effort thrombosis is still a problem because of missing approved treatment quidelines. Anticoagulation is the basis of the management of UEDVT with the main objective of preventing further propagation of thrombus. Consensus statements advocate catheter-directed thrombolysis within five days of symptoms. Hence, if there is evidence of thoracic outlet compression on imaging or symptomatic venous stenosis, consensus opinion advocates thoracic outlet decompression. The physicians are advised to use unfractionated heparin or low molecular weight heparin as initial step in DVT therapy followed by the acenocoumarol therapy. The current standard is six months of oral anticoagulation. [4] [12] In this case, patient experienced PE with low risk and was administered the same treatment as treatment for UEDVT i.e. low molecular weight heparin as initial step, followed by acenocoumarol therapy for six months. [13] After six months the patient was referred for thoracic outlet decompression. A review and treatment algorithm for Paget-Schröetter syndrome has recently been published. [14] | ||||||
|
Conclusion
| ||||||
|
Pulmonary embolism presenting with pleural effusion is difficult to diagnose. Asymptomatic subclavian vein thrombosis as source of embolus can be overlooked. Physicians and other health care professionals must be vigilant with young healthy individuals who have pleural effusion, because this symptom may be a 'forgotten sign' of life-threatening pulmonary embolism. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions:
Margita Belicová - Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Hubert Poláček - Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission:
The corresponding author is the guarantor of submission. |
|
Source of support:
None |
|
Conflict of interest:
Authors declare no conflict of interest. |
|
Copyright:
© Margita Belicová et al. 2012; This article is distributed the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any means provided the original authors and original publisher are properly credited. (Please see Copyright Policy for more information.) |
|
|