| Table of Contents |  |
|
Case Report
|
| Laparoscopic tubo-ovarian transposition prior to chemoradiation for uterine cervical cancer |
| Masaki Mandai1, Noriomi Matsumura2, Kenzo Kosaka3, Koji Yasumoto2, Tsukasa Baba2, Yumiko Yoshioka2, Ayako Suzuki2, Ikuo Konishi4 |
|
1Associate Professor, Department of Gynecology and Obstetrics Kyoto University Graduate School of Medicine, 54 Shogoin Kawahara-cho, Sakyo-ku, Kyoto 606-8507, Japan.
2Assistant Professor, Department of Gynecology and Obstetrics Kyoto University Graduate School of Medicine, 54 Shogoin Kawahara-cho, Sakyo-ku, Kyoto 606-8507, Japan. 3Medical Staff, Department of Gynecology and Obstetrics Kyoto University Graduate School of Medicine, 54 Shogoin Kawahara-cho, Sakyo-ku, Kyoto 606-8507, Japan. 3Professor, Department of Gynecology and Obstetrics Kyoto University Graduate School of Medicine, 54 Shogoin Kawahara-cho, Sakyo-ku, Kyoto 606-8507, Japan. |
|
doi:10.5348/ijcri-2012-06-137-CR-10
|
|
Address correspondence to: Masaki Mandai, M.D., PhD Associate Professor, Department of Gynecology and Obstetrics Kyoto University Graduate School of Medicine 54 Shogoin Kawahara-cho Sakyo-ku, Kyoto 606-8507 Japan Phone: [81]-75-751-3269 Fax: [81]-75-761-3967 Email: mandai@kuhp.kyoto-u.ac.jp |
|
[HTML Abstract]
[PDF Full Text]
|
| How to cite this article: |
| Mandai M, Matsumura N, Kosaka K, Yasumoto K, Baba T, Yoshioka Y, Suzuki A, Konishi I. Laparoscopic tubo-ovarian transposition prior to chemoradiation for uterine cervical cancer. International Journal of Case Reports and Images 2012;3(6):42–45. |
|
Abstract
|
|
Introduction:
Laparoscopic ovarian transposition is an effective method to preserve ovarian function in cancer patient who undergos pelvic irradiation. However, in usual operative procedure, the patients lose an ability to conceive naturally.
Case Report: We report a case of stage IIb uterine cervical cancer in which we performed a modified procedure of ovarian transposition. In an attempt to preserve potential ability for natural conception, we mobilized the fallopian tubes along with the ovaries by keeping the mutual proximity. Ovaries were anchored to the peritoneum outside the irradiation field. Conclusion: The procedure was safely performed under laparoscopy, and may be useful as a standard surgical procedure for the patients who desire preservation of fertility. | |
|
Key Words:
Ovarian transposition, Laparoscopy, Ovarian function, Fertility preservation
| |
|
Introduction
| ||||||
|
In the treatment of cancer in young women, one of the critical issues is the preservation of fertility. In treatment involving anti-cancer reagents, the use of drugs that are known to be less toxic to the ovary and the inhibition of ovulation using a GnRH agonist are thought to preserve fertility to some extent. If pelvic irradiation is considered in a young woman, the most realistic and effective method with which to preserve ovarian function is the surgical transposition of the ovaries. This method involves moving the ovaries outside the irradiation field while retaining ovarian circulation by preserving ovarian vessels. Ovarian transposition reduces the radiation dose to approximately 5% to 10% of the dose to the ovaries in their normal position. [1] This technique has been used in various malignancies, such as Hodgkin's disease, [2] ependymoma, [3] anal canal cancer [4] and uterine cervical cancer. [5] The procedure was previously performed by laparotomy. However, in recent years, a laparoscopic procedure has been reported, and the technique may become standard in the future, providing a minimally invasive means to preserve ovarian function. Nevertheless, patients who undergo ovarian transposition permanently lose the ability to conceive naturally. The only possible approach to conception in these women is to undergo IFV-ET, which may be more difficult than usual, because the ovaries are transposed outside the pelvis and transvaginal egg retrieval is impossible. In 1998, Tulandi et al. reported a laparoscopic procedure in which they transposed ovaries with fallopian tubes without transecting the tube. [6] Although it is theoretically a better procedure for sparing fertility, there are few reports on this procedure. Here, we report a case in which we performed the procedure under laparoscopy. | ||||||
|
Case Report
| ||||||
|
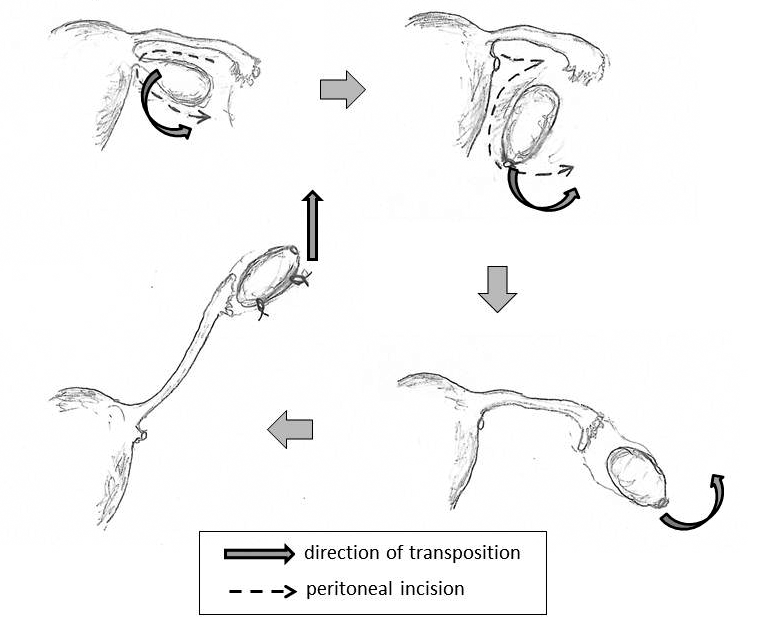
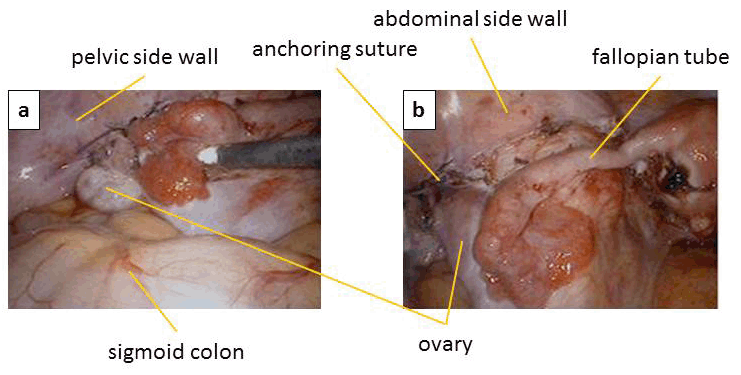
A 32-year-old nulliparous female was referred to our hospital with a diagnosis of invasive cervical cancer. Upon vaginal inspection, the uterine cervix was fragile and carcinomatous. The anterior vaginal fornix was involved and apparent parametrial invasion was observed. The mass measured six cm in diameter on MRI. Pathology revealed invasive papillary squamous cell carcinoma. We proposed radical hysterectomy or concurrent chemoradiation (CCRT) as treatment options, and the patient chose CCRT. She strongly valued the preservation of ovarian function and of fertility. Therefore, we recommended laparoscopic ovarian transposition by the modified procedure as described below. Ovarian transposition was performed according to the method described by Tulandi et al. [6] We used three trocar ports and a camera port in the umbilicus. There was no apparent adhesion in the abdominal cavity. No apparent malignant finding such as dissemination was noted. Peritoneal lavage cytology was negative. The operation was initiated by dividing the left ovarian ligament using a Ligasure (Covidien, Tokyo, Japan). Then, the mesovarium was electrocoagulated and incised to separate the left ovary from the fallopian tube while maintaining the proximity between the fimbria and the ovary (Figure 1). The peritoneum was continuously incised along the line of the ovarian vessels to move the ovary. After adequate mobilization, the left ovary was lifted up to the level of the anterior-superior iliac spine. The ovary was then anchored to the peritoneum on the psoas muscle with two sutures of 3-0 proline (nylon). The same procedures were performed on the right side (Figure 2). The ovaries were marked with metal clips. Blood loss was minimal. The patient underwent CCRT starting one week after surgery. She received a total of 50.4 Gy of whole-pelvic radiation and 10 Gy of brachytherapy, along with six courses of concurrent 40 mg/m2 cisplatin administration. She has just finished the treatment. Notably, the patient also menstruated during the treatment. | ||||||
| ||||||
| ||||||
|
Discussion
| ||||||
|
Increasingly younger patients are reported to suffer from uterine cervical cancer. One of the obstacles of treatment for invasive cervical cancer is the loss of fertility. For patients with early invasive cervical cancer, radical trachelectomy is becoming a new standard modality in patients who strongly desire to preserve their fertility. Even in cases that do not require fertility, a surgical procedure such as radical hysterectomy without bilateral oophorectomy can preserve ovarian function in young patients. In contrast, if patients undergo radiation therapy, fertility and ovarian function are compromised unless a special surgical procedure, an ovarian transposition, is performed. In recent years, a laparoscopic procedure for ovarian transposition has been reported and the technique may become standard in the future, providing a minimally invasive means of preserving ovarian function. [7] There are several reports on successful pregnancy after the transposition of the ovaries. Pahisa et al. performed ovarian transposition in 28 FIGO-stage IB1 cervical cancer patients who were younger than 46 years and 12 patients who underwent pelvic radiotherapy. [5] At a mean follow-up of 44 months, more than 60% of the irradiated patients exhibited normal ovarian function. In a report by Morice et al. 15 out of 19 (79%) patients who received postoperative irradiation exhibited preserved ovarian function. [7] Bloemers et al. reported a case in which chemo-radiation was employed as treatment. [8] The patient had normal menstrual cycles at regular monthly intervals after more than three years had elapsed since the initial treatment. Several cases of surrogate pregnancy were reported in patients with preserved ovaries, suggesting that this procedure also preserves fertility. [9] [10] However, natural conception is impossible after a transposition. Tulandi et al. reported a modified ovarian preservation procedure, in which the fimbria portion was transposed along with the ovary without transecting the fallopian tubes. [6] This procedure retains anatomical proximity between the ovary and fimbria of the fallopian tube, thereby preserving the ability to conceive naturally. The authors observed one case of natural conception and the delivery of a healthy infant after pelvic irradiation for rectal carcinoma. [11] In addition, recently, Ferrari et al. reported a case of spontaneous conception and uneventful vaginal delivery in a patient who underwent this procedure prior to irradiation for B-cell lymphoma. [12] As we report in the case presentation, this procedure is easily and safely performed by laparoscopy. Therefore, we strongly recommend this procedure for patients in whom ovarian transposition is indicated, who strongly desire to remain fertile. However, since there are few reports on the outcome of this procedure, further research is necessary to conclusively determine the effects of this procedure on pregnancy. | ||||||
|
Conclusion
| ||||||
|
Transposition of both ovaries and fallopian tubes may be used as a standard operative procedure for cancer patient who wish for preservation of fertility. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions:
Masaki Mandai - Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Noriomi Matsumura - Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Kenzo Kosaka - Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Koji Yasumoto - Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Tsukasa Baba - Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Yumiko Yoshioka - Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Ayako Suzuki - Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Ikuo Konishi - Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission:
The corresponding author is the guarantor of submission. |
|
Source of support:
None |
|
Conflict of interest:
There is no conflict of interest regarding this article in any of the authors. |
|
Copyright:
© Masaki Mandai et al. 2012; This article is distributed the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any means provided the original authors and original publisher are properly credited. (Please see Copyright Policy for more information.) |
|
|