| Table of Contents |  |
|
Case Series
|
| Versatility of limberg flap in head and neck region |
| Abdul Ahad G Khan1, Kanchan M Shah2 |
|
1Assistant professor, Dept. of Oral and Maxillofacial Surgery, Govt. Dental College and Hospital, Aurangabad, Maharashtra, India.
2Associate professor & Head of Department, Dept. of Oral and Maxillofacial Surgery, Govt. Dental College and Hospital, Aurangabad, Maharashtra, India. |
|
doi:10.5348/ijcri-2012-06-130-CS-3
|
|
Address correspondence to: Dr. Abdul Ahad Khan, MDS (Oral and Maxillofacial Surgery) Plot no. A-1, Gut no. 13, Opposite Amber Gas Godown, Nasik Road Padegaon, Aurangabad Maharashtra India - 431002 Phone: 9552002731, 9324107926 Email: drabdulahadkhan@gmail.com, drabdulahadkhan09@rediff.com |
|
[HTML Abstract]
[PDF Full Text]
|
| How to cite this article: |
| Khan AAG, Shah KM. Versatility of limberg flap in head and neck region. International Journal of Case Reports and Images 2012;3(6):13–18. |
|
Abstract
|
|
Introduction:
The rhomboid flap was introduced by Professor AA Limberg of Leningrad, hence also called as the Limberg flap. It is an interesting procedure for skin movement in which a rhomboid defect is created and then closed with a rhomboid shaped flap of a similar size. The surgeon's goal is to avoid unsightly scars while using the simplest, most effective reconstructive approach.
Case Series: The present paper demonstrates the versatility of the rhomboid flap in head neck region. Two cases, one of dento-alveolar infection and the other of cervicofacial actinomycosis are presented, in which the unsightly scars that could have been produced by excision of the lesion alone, has been avoided by the use of rhomboid flap. Conclusion: Rhomboid flap is a very versatile and robust flap, easy to master and practice, that can be tailored to suit the surgeon's needs. | |
|
Key Words:
Limberg, Rhomboid, Local flap
| |
|
Introduction
| ||||||
|
The face and its features have been the subject of poetic and artistic endeavors throughout the ages. Because a person's face is highly visible and difficult to camouflage, any scars or imperfections are obvious to others and may be distressing to the affected individual. Particular skill is required of the surgeon reconstructing facial defects because the cosmetic result will have physical and psychological implications for the patient. The surgeon's goal is to avoid unsightly scars while using the simplest and most effective reconstructive approach. [1] Professor Limberg devoted his entire career to flap design, publishing first on the subject in 1928. His first treatise in English was a chapter in Modern Trends in Plastic Surgery, edited by Thomas Gibson of Glasgow University (Glasgow, Scotland) in 1963. [2] In that chapter, he outlined his rhomboid flap. The rhomboid flap can be used to close defects almost anywhere on the body. It is versatile in that a random pattern flap can be raised from any one or all corners of the rhomboid. The defect is filled with tissue of the same thickness and colour, and with good vascularity. [3] | ||||||
|
Case Series
| ||||||
|
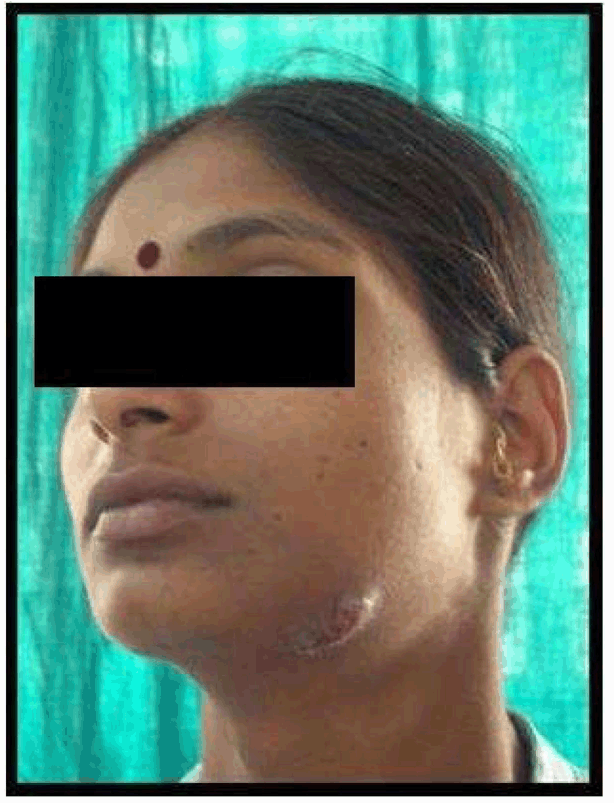
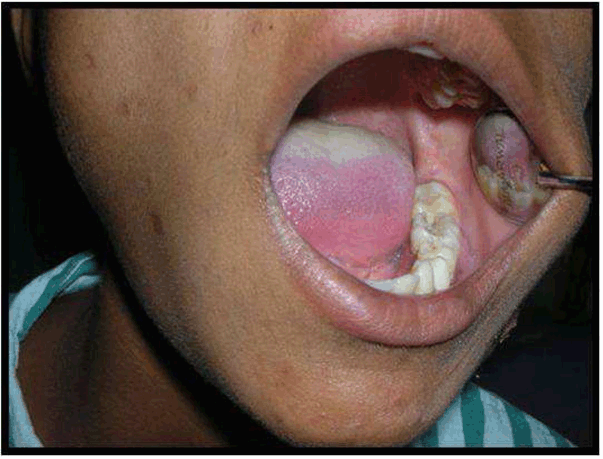
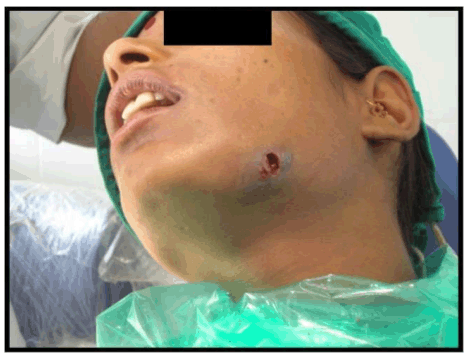
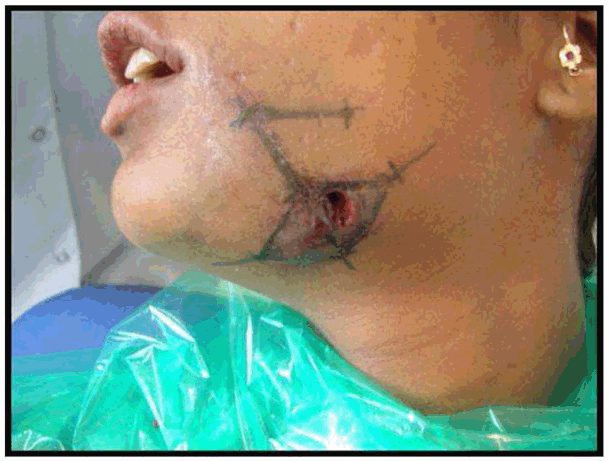
Case No. 1: A 28-year-old lady, was referred to our department with the complaint of extra-oral draining sinus over left submandibular region secondary to an infected left mandibular 1st molar. She had history of recurrent pain and swelling over the left submandibular region since about eight months for which she used to take medicines from the pharmacy shop without consulting any doctor. The present episode resulted in a sinus through which pus was draining. She was also experiencing paresthesia over left half of lower lip. The medical history was not contributory. On clinical examination left mandibular 1st molar was carious and tender to vertical percussion. Lateral oblique radiographic view of left side of mandible revealed a radiolucent lesion in connection with left mandibular 1st molar extending upto the inferior alveolar canal region. Blood reports were within the normal range except for an elevated ESR. Under all aseptic precautions and antibiotic cover, the offending tooth was extracted, the periapical area was curetted with bone curettes and the sinus track was curetted by means of tape/roller gauze soaked in povidone-iodine (by to and fro motion). As the wound could not be closed primarily and secondary healing would have produced a depressed scar, so it was planned to do a rhomboid flap to close the defect by advancing adjacent tissue. Unfortunately the patient did not return for follow up so the post-operative photographs could not be recorded (Figures 1–7). | ||||||
| ||||||
|
| ||||||
| ||||||
|
| ||||||
| ||||||
|
| ||||||
| ||||||
|
| ||||||
| ||||||
|
| ||||||
| ||||||
|
| ||||||
| ||||||
|
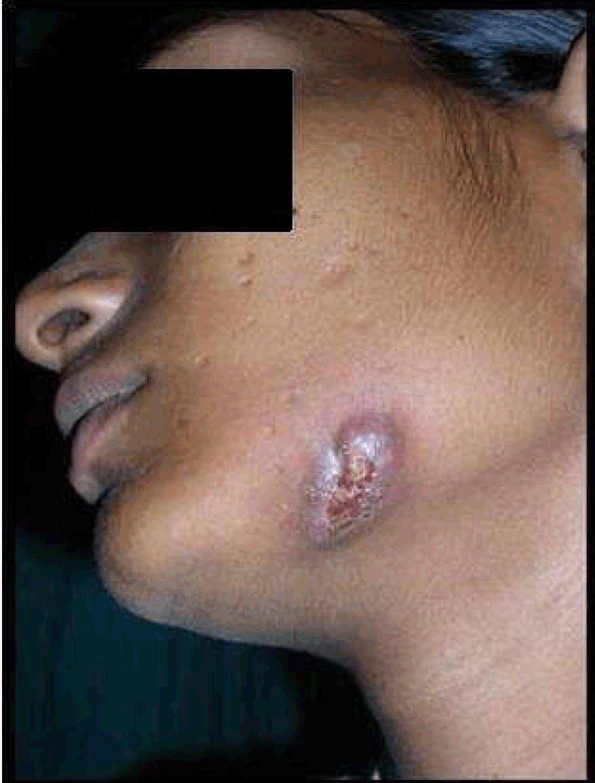
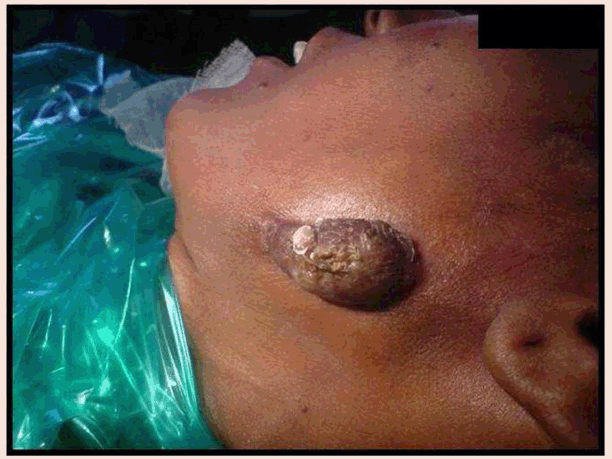
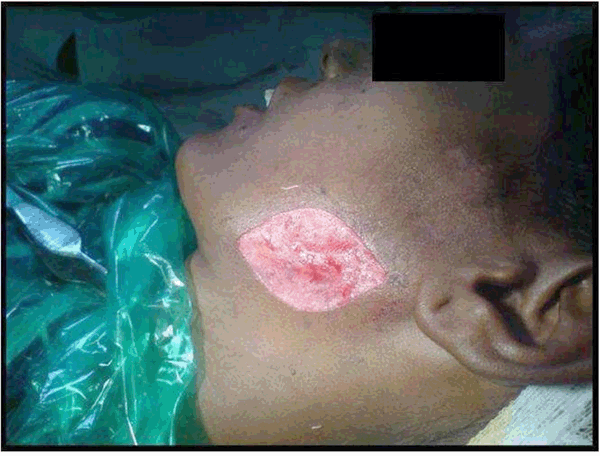
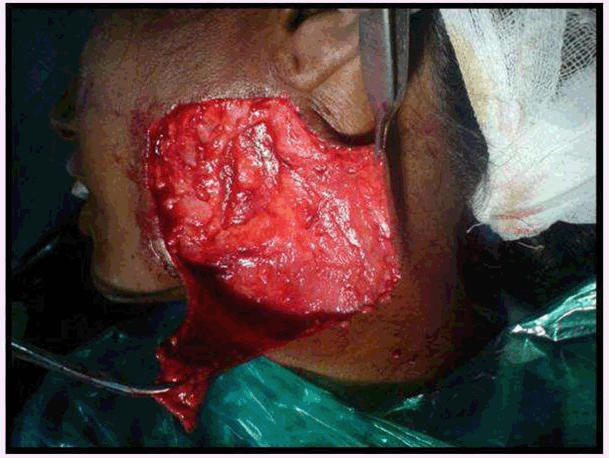
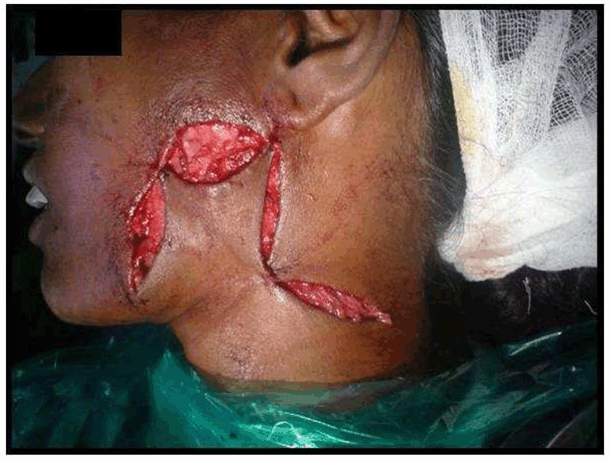
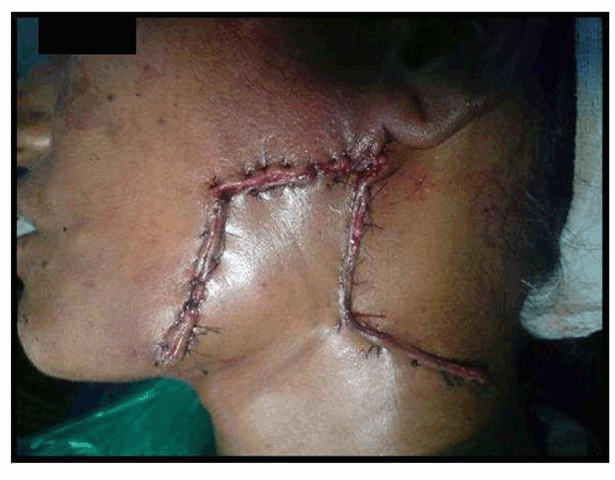
Case No. 2: A 35-year-old lady was referred to our department with the complaint of an ugly looking growth over the skin of left angle region of the mandible. She had history of extraction of lower left first molar six months back. One month later, a swelling with pus discharging sinus appeared in the pre-auricular area which subsided on taking medications. Thereafter, the swelling reappeared and subsided many times. The present swelling had appeared 1 ½ months back. The medical history was not contributory. On clinical examination, a reddish brown, firm, swelling with irregular scarred surface, of approximately 3x2 cm was present on the skin overlying left mandibular ramus. There was no odontogenic cause evident and radiographs showed no abnormality. FNAC was also not conclusive. CT scan revealed the lesion was only skin deep showing no evidence of underlying bone erosion so it was planned to excise the mass in total and then send the lesion for histopathology. As the residual defect was big enough for primary closure, it was planned to reconstruct with a rhomboid flap by mobilization of adjacent tissue, under all aseptic precautions and under antibiotic cover. Clinical, radiological and histopathological correlation of the mass lead to the diagnosis of cervicofacial actinomycosis (Figures 8–13). | ||||||
| ||||||
|
| ||||||
| ||||||
|
| ||||||
| ||||||
|
| ||||||
| ||||||
|
| ||||||
| ||||||
|
| ||||||
| ||||||
|
Discussion
| ||||||
|
Rhomboid flap is an interesting procedure for skin movement in which a rhomboid defect is created and then closed with a rhomboid shaped flap of a similar size. It is basically a parallelogram with two angles of 120° and two of 60°. These angles, of course, can be modified depending on the shape of the lesion or defect. All sides of the rhomboid and all sides of the flap are equal. As many as four flaps can be raised from one rhomboid, if required. A literature search turned up 54 articles on the use of the rhomboid (Limberg) flap in all areas of the body and by several surgical specialties. There are nine articles on its use for pilonidal sinus and three for hand surgery, as well as several examples of its use in ophthalmology and otolaryngology. This flap is obviously an attractive choice in many body areas. It has special application for eyelid, floor of nose, alar rim and chin defects. It is proposed that the rhomboid (Limberg) flap, single or multiple, can be applied widely with extreme safety and good cosmetic results. It is a transposition flap that, like the bilobed flap and the Z-plasty, depends on the pliability of the adjacent skin, which can be determined by pinching various areas between the thumb and forefinger. [5] The technique of its elevation is simple. The elevated flap requires sufficient subcutaneous fat, and dissection must be carried past its base to prevent an elevated bump when it is transposed. In designing a rhomboid flap, the surgeon draws a line from the outer point of the 120° angle; this line bisects the angle, with its length being equal to that side of the rhomboid. From the outer point of this line, another line is drawn at 60° parallel to the side of the rhomboid defect. Its length again equals that of the side of the rhomboid. Before any incisions are made a further check of skin availability is made with thumb and forefinger. This checking procedure ensures that the donor defect will close. If it will not, the original rhomboid may be changed in position or another donor flap can be used. [1] The crucial point in designing a Limberg flap is the correct placement of the direction of the base of triangle in relation to the line (axis) of maximum extensibility. The latter is at a right angle to the relaxed skin tension line. [4] An additional consideration is the position of the donor defect; it should lie, if possible, in the long axis of a line of minimal tension. Its closure should not distort local anatomic features such as hairline or eyebrow. As depicted in (Figure 14A), four potential flaps can be designed for each rhomboid. Using the principles outlined here, the surgeon chooses the most convenient one. The excision is completed and the donor flap is elevated (Figure 14B). As with the Z-plasty, this elevation should extend slightly beyond the base of the flap (Figure 14C). The excisional defect is usually closed without difficulty. The angles of the flap are fixed by three-point sutures. The donor site is closed directly (Figure 14D). [6] The Dufourmentel flap technique, described by Dufourmentel in 1962, is a modification of the rhomboid flap. It is somewhat complex, that undoubtedly provides more tissue to close the defect than is absolutely necessary, thus can be used in certain situations, when a rhomboid flap may give difficulty in donor site closure, but needs experience to master the technique. [1] | ||||||
|
| ||||||
|
Conclusion
| ||||||
|
Rhomboid flap is a very versatile, easy to master flap that can be applied with extreme safety and can be tailored to suit the surgeon's needs. As there is abundance of subcutaneous tissue in the face, it can be easily used to correct small to medium sized defects with good cosmetic results. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions:
Abdul Ahad G Khan - Conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Critical revision of the article, Final approval of the version to be published Kanchan M Shah - Conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Final approval of the version to be published |
|
Guarantor of submission:
The corresponding author is the guarantor of submission. |
|
Source of support:
None |
|
Conflict of interest:
Authors declare no conflict of interest. |
|
Copyright:
© Abdul Ahad G Khan et al. 2012; This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any means provided the original authors and original publisher are properly credited. (Please see Copyright Policy for more information.) |
|
|