| Table of Contents |  |
|
Case Report
|
| A case of primary orbital neuroblastoma |
| Rayees Ahmad Sofi1, Sajad Bashir Khanday1, Manzoor Qadir Keng1, Junaid Salam Wani1, Ankur Goel1, Tufaila Shafi1 |
|
1Department of ophthalmology, Government Medical College, Srinagar, India.
|
|
doi:10.5348/ijcri-2012-03-100-CR-5
|
|
Address correspondence to: Rayees Ahmad Sofi House no. - 134, Lane no. 2 , Sir Syed Colony Upper Soura Srinagar Jammu and Kashmir, 190002 India Phone: +919419070838 Email: rayees630@yahoo.co.in |
|
[HTML Abstract]
[PDF Full Text]
|
| How to cite this article: |
| Sofi RA, Khanday SB, Keng MQ, Wani JS, Goel A, Shafi T. A case of primary orbital neuroblastoma. International Journal of Case Reports and Images 2012;3(3):16-18. |
|
Abstract
|
|
Introduction:
Neuroblastoma is a pediatric neoplasm that is most common cancer diagnosed during infancy. Male to female ratio is 1.1:1 showing slight preponderance towards males. Neuroblastoma occurs primarily in the abdomen in 60% cases but in 8% cases the tumour arises in the orbit where it arises from ciliary ganglion. Seventy-five percent cases occur before the age of four years.
Case Report: We describe a case of five year old boy who presented with a rapidly progressing large tumour in his left orbit. CECT revealed a mass in the left orbital region pushing the eyeball anteriorly. A histopathologic diagnosis of neuroblastoma was made. Subsequent medical evaluation including chest X-ray, USG of the abdomen, whole body computerized tomography and bone scintigraphy showed no evidence of systemic involvement or metastasis. Conclusion: Neuroblastoma although an uncommon primary orbital tumour in children but it should be considered in the differenrial diagnosis of orbital tumours in children. | |
|
Key Words:
Primary, Orbital, Neuroblastoma, Child
| |
|
Introduction
| ||||||
|
Neuroblastoma is an undifferentiated malignant tumour of the primitive neuroblasts. Neuroblastoma is a pediatric neoplasm that is most common cancer diagnosed during infancy. [1] [2] Male to female ratio is 1.1:1 showing slight preponderance towards males. [3] Neuroblastoma occurs primarily in abdomen in 60% cases but in 8% cases the tumour arises in the orbit where it arises from ciliary ganglion. Seventy-five percent of cases occur before the age of four years. Primary orbital neuroblastoma has been reported previous in adults [2] and neonates. [4] | ||||||
|
Case Report
| ||||||
|
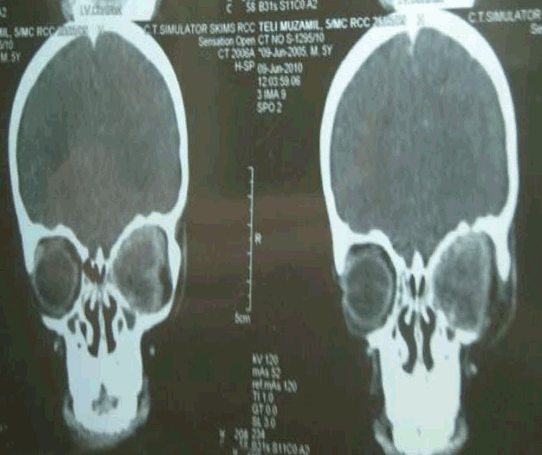
A 5-year-old boy was brought to the Outpatient Department of our hospital with complaints of painless, rapidly progressing protrusion of the left eye since five months which was associated with loss of vision. The mass between the lids was red and firm in appearance and impeded any view of his left globe (figure 1). Patient was physically normal and had no signs of congenital malformation. There were gross restriction in movement of proptosed mass in all positions of gaze. Symblepharon was present. No, other details could be seen. The lids were oedematous and ecchymosed. The mass was non-tender and globular. It was immobile and non pulsatile. It was not expansible on coughing or crying. Right eye appeared normal. Investigations: Complete hemogram, including general blood picture, ESR, urine and stool examination were found to be within normal limits. Computed tomography (CT) scan showed soft tissue density enhancing mass in the left retro-orbital region measuring 3x2.7 cm pushing the left eye ball anteriorly. The optic nerve could not be separated out and lesion seemed to be adherent to the eye ball. There was no evidence of mass in the sinuses, nasal cavities or intra- cranial cavities (figure 2). Ultrasomography (USG) scan of the left eye ball was performed using high frequency and showed a large hypoechoic mass. Fine needle aspiration cytology (FNAC) of the tissue showed features suggestive of Neuroblastoma. Excision biopsy on histopathological examination showed tumour consisting of small round cells with high mitotic activity in a neurofibrillary and haemorrhagic background. The tumour cells were forming Homer - Wright pseudorosetts. Some sites showed haemorrhagic necrosis (figure 3). The tumour cells were positive for synaptophysin, neuron specific enolase, chromogranin and focally for glial fibrillary acidic protein. A histopathological diagnosis of neuroblastoma was made. Subsequent medical evaluation including chest X-ray, USG of the abdomen, whole body CT scan and bone scintigrapy showed no evidence of systemic involvement or metastasis. Tumour was diagnosed as primary orbital neuroblastoma. The whole orbital exenteration operation was done under general anesthesia and the patient further received 11 cycles of chemotherapy and 36 Gy local EBRT. Adequate treatment was given and patient was further referred to pediatric oncology department for further management. | ||||||
| ||||||
| ||||||
| ||||||
|
Discussion
| ||||||
|
Neuroblastoma is an undifferentiated malignant tumour of primitive neuroblasts which may be metastatic to the orbit. It represents second most common orbital tumour in children after rhabdomyosarcoma. It arises from the sympathetic system and ganglia and represents the peripheral nervous system counter part of retinoblastoma. Rarely neuroblastomas may represent primary lesions in the orbit where they may arise from ciliary ganglion. [5] Only 8% cases first present with an orbital lesion; in 92% of cases the presence of extra orbital primary tumour is already known. [5] Fourty percent of orbital lesions are bilateral. Mean age at presentation is two-years-old. [5] 75% of cases occur before the age of four years. [5] Commonly there is bone destruction particularly of lateral orbital wall. Ten to fourty percent of systemic neuroblastomas result in orbital metastasis within three months after diagnosis. Fourty percent of orbital metastasis are bilateral. Other possible ophthalmic manifestations of metastatic neuroblastomas are horner's syndrome, papilledema, retinal striae, anisocoria, nystagmus and cranial nerve paralysis. About 90% of orbital lesions originate from abdomen. [6] [7] [8] Histopathologically other small round cell tumours especially non-hodgkin's lymphomas and rhabdomyosarcomas must be taken into consideration for differential diagnosis of neuroblastoma. [4] The pathological features and immunohistochemistry certainly pointed out to the neuroblastoma in our case. Further-more the systemic examination ruled out any other primary lesion or metastatic foci pointing this to be the case of primary orbital neuroblastoma. The primary orbital neuroblastoma is definitely a rare case presentation. Till now very few cases of primary orbital neuroblastoma have been reported. [1] | ||||||
|
Conclusion
| ||||||
|
Neuroblastoma although an uncommon primary orbital tumour in children should be considered in the differenrial diagnosis of orbital tumours in children. | ||||||
|
Acknowledgements
| ||||||
|
We are thankful to Dr. Ghulam Nabi Sofi, Additional Professor, Pathology, for histopathological analysis and Junaid Nabi, extern medical student for his valuable suggestions and support. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions:
Rayees Ahmad Sofi - Substancial contribution to the conception and design, acquisition of data, analysis and interpretation of data, drafting the article, revising it critically for important intellectual content, final approval of data Sajad Bashir Khanday - Substancial contribution to the conception and design, analysis and interpretation of data, drafting the article, revising it critically for important intellectual content, final approval of data Manzoor Qadir Keng - Substancial contribution to the conception and design, revising it critically for important intellectual content and final approval of version to be published Junaid Salam Wani - Analysis and interpretation of data, revising it critically for important intellectual content, final approval of version to be published Ankur Goel - Acquisition of data, drafting the article, revising it critically for important intellectual content, final approval of data Tufaila Shafi - Acquisition of data, revising it critically for important intellectual content, final approval of the version to be published |
|
Guarantor of submission:
The corresponding author is the guarantor of Submission. |
|
Source of support:
None |
|
Conflict of interest:
The authors declare no conflict of interest. |
|
Copyright:
© Rayees Ahmad Sofi et al. 2012; This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any means provided the original authors and original publisher are properly credited. (Please see http://www.ijcasereportsandimages.com/copyright-policy.php for more information.) |
|
|