|

|
 |
|
Case Report
| ||||||
| Emphysematous gastritis after bone marrow transplant: Successful conservative management | ||||||
| Hammad Liaquat1, Imad Jaafar2, Matt Bojanowski3, Endashaw Omer4 | ||||||
|
1MD, Gastroenterology Fellow, Division of Gastroenterology, Hepatology and Nutrition, Department of Internal Medicine, University of Louisville, Louisville, Kentucky, USA.
2MD, Medical Resident, Department of Internal Medicine, University of Louisville, Louisville, Kentucky, USA. 3Medical Students, School of Medicine, University of Louisville, Louisville, Kentucky, USA. 4MD, Assistant Professor of Medicine, Division of Gastroenterology, Hepatology and Nutrition, Department of Internal Medicine, University of Louisville, Louisville, Kentucky, USA. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Liaquat H, Jaafar I, Bojanowski M, Omer E. Emphysematous gastritis after bone marrow transplant: Successful conservative management. Int J Case Rep Images 2016;7(7):454–457. |
|
Abstract
|
|
Introduction:
Emphysematous gastritis (EG) has a nonspecific presentation, so radiography is an essential diagnostic tool. There is usually a high mortality rate and poor prognosis associated with EG.
Case Report: A 38-year-old male with a history of recurrent seminoma who received chemotherapy and underwent stem cell transplantation before he was diagnosed with EG. During the hospital course, the patient developed gastrointestinal symptoms, neutropenic fever and, subsequently, multi-organ failure. Medical imaging reported findings consistent with EG. The patient was managed conservatively with subsequent recovery and resolution of EG on repeat medical imaging. Conclusion: Emphysematous gastritis in the setting of immunosuppression and multi-organ failure can be managed successfully with prompt diagnosis and conservative management. | |
|
Keywords:
Bone marrow transplant, Conservative management, Emphysematous gastritis, Multi-organ failure
| |
|
Introduction
| ||||||
|
Emphysematous gastritis (EG) is the presence of gas within the stomach wall in association with clinical sepsis [1]. Initially reported in 1889 by Fraenkel, EG is a rare illness diagnosed with the support of imaging and is associated with mortality rate reported to be as high as 62%. Approximately 70 cases of EG have been reported in literature so far. There are some reports of successful conservative management in uncomplicated EG while surgery is usually required in the presence of complications like perforation or peritonitis [2]. We present a case of a man with testicular cancer who developed EG after recent chemotherapy and stem cell transplantation and was managed successfully with conservative treatment. | ||||||
|
Case Report
| ||||||
|
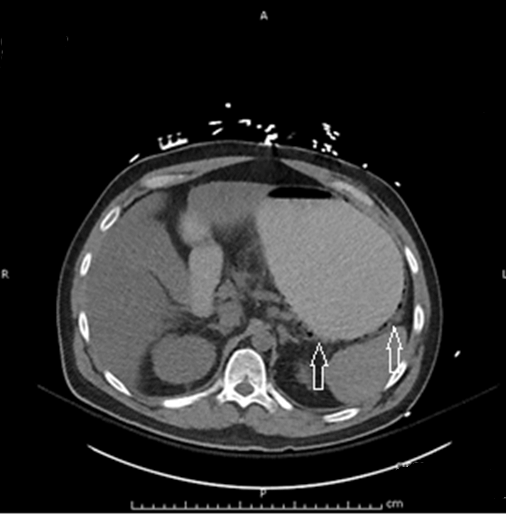
A 38-year-old male with a history of relapsed seminoma was admitted to the University Hospital for autologous stem cell transplantation after he had received several cycles of neoadjuvant chemotherapy. One day after successful bone marrow transplant he developed nausea, vomiting, abdominal pain and diarrhea. Subsequently, he developed fever with daily temperature spikes of 102–105°F. He became progressively pancytopenic and, three days after stem cell transplant, his absolute neutrophil count reached nadir of 100 cells per microliter. Patient continued to deteriorate clinically and developed multi-organ failure. He was put on mechanical ventilation, given intravenous fluid resuscitation and broad spectrum antibiotics empirically (meropenem, vancomycin, micafungin and acyclovir). His renal function continued to worsen and hemodialysis was initiated. All infectious workup was negative except for a positive cytomegalovirus IgM antibody. Plain film of the chest did not show pneumonia. His gastrointestinal symptoms continued to worsen. A CT scan of the abdomen without contrast revealed diffuse pneumatosis of the stomach consistent with a diagnosis of EG (Figure 1). No portal venous gas or free intraperitoneal air was seen on CT scan. The surgery consult service was consulted and they recommended medical management. He received intravenous hydration, total parenteral nutrition, bowel rest and gastric decompression with nasogastric tube. The patient was monitored with daily plain films of the abdomen. Antiviral therapy was switched to ganciclovir. After three weeks of conservative therapy, the patient's clinical status began to improve. His abdominal pain and diarrhea resolved, and gastric output was negligible. Serial plain films of the abdomen showed decreasing distension of the stomach and small bowel. He was successfully extubated, and the nasogastric tube was removed. The patient continued to recover well clinically and lab abnormalities resolved. His diet was advanced slowly, which was well tolerated. A repeat abdominal CT scan reported resolution of EG (Figure 2). He was later discharged from the hospital with instructions for outpatient oncology, nephrology and gastroenterology follow-up. The patient was seen in gastroenterology clinic two weeks after discharge from the hospital. He had no gastrointestinal complaints, had normal bowel function and was eating a normal diet. His blood electrolytes and cell counts continued to be within normal range. | ||||||
|
| ||||||
| ||||||
|
Discussion
| ||||||
|
Emphysematous gastritis is often associated with conditions that damage the gastric mucosal barrier and thus enable bacteria to establish themselves in this unusual location. Known associated conditions include ingestion of corrosives, alcohol abuse, renal failure, diabetes, non-steroidal anti-inflammatory drug usage, pancreatitis, gastroenteritis and recent abdominal surgery [2][3] There have been cases of associated bacterial infection with Clostridium welchii, Escherichia coli, Streptococcus, Bacillus subtilis, proteus, Pseudomonas and Enterobacter [1] [4] . Our patient was immunosuppressed, developed renal failure and tested negative on all bacterial cultures. There is no established diagnostic criteria for EG [2]. Previous studies have suggested severe symptoms, characteristic medical imaging and bacterial infection as diagnostic markers. The clinical course and medical imaging in our patient was characteristic of EG. Typically, gas is unusual within the stomach due to its mucosal barrier, acidity, and strong blood supply [3] [4]. It can be a sign of underlying disease and is found in EG as well as gastric emphysema. Gastric emphysema (GE) is usually associated with an asymptomatic clinical course without co-existent microbial infection and early spontaneous resolution [5] [6]. Severe clinical illness and co-morbidity, microbial infection usually with gas-forming bacteria, and high mortality rate are hallmarks of EG. There is also a greater likelihood for the need of surgery in a patient with EG [7]. Computed tomography scan of the abdomen is the best imaging modality to differentiate between GE and EG. Characteristic circular air bubbles are found in GE, while thickened gastric folds along with linear streaks of air are found in EG. The presence of portal venous gas can also be found with EG and is usually concerning for development of mesenteric ischemia [3]. Our patient underwent stem cell transplant prior to his presentation of EG. This may be the first reported case of a patient who developed EG after autologous stem cell transplant. A case in Korea has developed gastric pneumatosis mimicking an intestinal perforation after hematopoietic stem cell transplantation, but he did not develop EG [8]. The most closely related report has been a case of a patient with aplastic anemia developing emphysematous gastritis [4]. Our patient also uniquely presented with a positive IgM result for cytomegalovirus (CMV). The CMV is the most commonly recognized viral infection of the stomach [9] but a past literature search does not show a case of emphysematous gastritis with CMV infection. Our patient may be the first reported case in this regard as well. There is no consensus about the optimal management of EG. Conservative medical management for EG has been successful in several cases [2] [4][10]. The management in these cases included bowel rest, hyperalimentation via central venous nutrition, broad-spectrum antibiotics, proton pump inhibitors and a nasogastric tube. Despite immunosuppression and multi-organ failure, our patient recovered with standard medical management. Some patients with similar co-morbidity have not survived similar management in the past [11] [12][13]. Surgical intervention has been successful for cases of EG complicated by gastric or intestinal perforation, ischemia, and unsuccessful medical management [4] [14][15]. | ||||||
|
Conclusion
| ||||||
|
Emphysematous gastritis is a rare and critical illness. It has non-specific presentation and has high mortality rate. Prompt diagnosis and conservative management can prevent complications and adverse outcome as well as result in complete recovery of patient. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Hammad Liaquat – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Imad Jaafar – Acquisition of data, Analysis and interpretation of data, Drafting the article, Final approval of the version to be published Matt Bojanowski – Acquisition of data, Analysis and interpretation of data, Drafting the article, Final approval of the version to be published Endashaw Omer – Substantial contributions to conception and design, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2016 Hammad Liaquat et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|