|

|
 |
|
Case Report
| ||||||
| Tetraplegia developing with skull traction in patients with ankylosing spondylitis: A case report | ||||||
| Emrullah Hayta1, Ahmet Karadağ1, Cesur Gumus2 | ||||||
|
1Assistant Professor, Cumhuriyet University, Faculty of Medicine, Deparment of Physical Medicine and Rehabilitation, Sivas, Turkey.
2Professor, Cumhuriyet University, Faculty of Medicine, Deparment of Radiology, Sivas, Turkey. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Hayta E, Karadag A, Gumus C. Tetraplegia developing with skull traction in patients with ankylosing spondylitis: A case report. Int J Case Rep Images 2016;7(2):111–114. |
|
Abstract
|
|
Introduction:
Traffic accidents appear to be one of the frequently encountered causes of spinal cord injury (SPI) in patients with ankylosing spondylitis. The risk of spinal cord injury is 11.4 times higher in patients with AS compared to the healthy population. Although the fractures might be seen in any part of the spine, they most frequently occur in cervical region.
Case Report: Our subject in this case is a 62-year-old patient diagnosed with AS who had isolated muscle strength loss following a traffic accident. The patient was provided skull traction treatment having sustained a fracture in his C7 in a traffic accident, and he developed tetraplegia as a result. Conclusion: Our objective with this case report is to emphasize that stress loading treatment methods such as skull traction which apply force to bone in fractures arising from traumas in patients with AS could lead to extremely severe neurological injuries. | |
|
Keywords:
Ankylosing spondylitis, Rehabilitation, Skull traction, Spinal cord injury
| |
|
Introduction
| ||||||
|
Ankylosing spondylitis (AS) is a chronic inflammatory disease characterized by enthesitis which specifically holds on sacroiliac joints, axial skeleton and sometimes on peripheral joints [1]. As a result of secondary osteoporosis and rigid spine with reduced mobility occurring in AS, the spine loses its elasticity and ability to counter impacts. Even the smallest load might easily lead to fractures in spine. The fact that pathology in cervical vertebrae might not be detected in conventional radiological examination might result in delayed diagnosis [2] [3]. In this case report, we present a subject with AS who sustained spinal cord injury (SCI) following skull traction implementation conducted due to cervical spinal cord injury in a traffic accident in a car. Our objective is to underline that stress loading treatment methods such as skull traction which apply force to bone in neurological complications arising from simple traumas in patients with AS might lead to extremely severe neurological injuries. | ||||||
|
Case Report
| ||||||
|
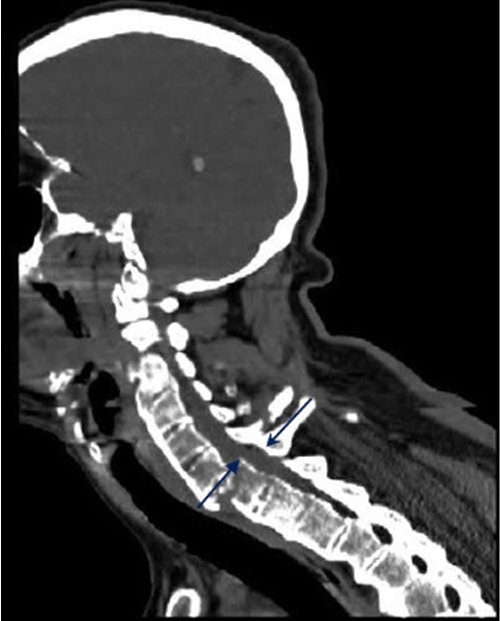
A 62-year old patient was admitted to our clinic complaining about walking problems and weakness in fingers of both hands. The patient history showed that he had been diagnosed with AS around 30 years ago, and used sulfasalazine and non-steroidal anti-inflammatory drugs due to this diagnosis. He had been admitted to hospital complaining about weakness in his right hand fingers resulting from a car accident. Computed tomography (CT) scan conducted in neurosurgery service showed a fracture in his C6-C7 vertebral corpus, posterior subluxation of C7 corpus and line in his spinous process C6, and he was recommended hospitalization for a clinical monitoring (Figure 1). On his second day in the hospital, he received a skull traction application for two hours after which a halo orthosis was mounted on him. Immediately after skull traction, the patient developed weakness (tetraplegia) in fingers of both extremities and bilateral lower extremities. Our clinic recommended consultation for the patient whose musculoskeletal examination showed anteflexion deformity in his cervical spine and thoracic kyphosis. The patient had 2.5 cm of thoracic expansion. Muscle strength examination showed that his right finger flexion was 2/5, and left finger flexion was 3/5, and finger abduction on the right was 2/5, and finger abduction on the left was 4/5, and bilateral lower extremity had the strength of 0/5. Sensory examination showed that left T4 had hypoesthesia starting from right T6, and anal sensation was positive. The patient did not have urinary or fecal incontinence. He had radiological level C/7, and his neurological level and C/7 functional independence measure (FIM) score was 55. Magnetic resonance imaging (MRI) scan of the patient indicated non-displaced fracture line in his vertebral corpus C7, and a non-displaced fracture line in his spinous process C6, and non-displaced fracture line in his vertebral facet joint level, spinal cord compression and edema signal (Figure 2). The patient was diagnosed with ASIA-B according to deformity scale by American Spinal Cord Injury Association (ASIA) as a result of the examination and radiological visualization. His neck was immobilized with a halo orthosis throughout his stay in the clinic. He was implemented tilt-table procedure in the acute period. As a part of rehabilitation program, we started to give the patient whole body range of motion exercises, exercises strengthening upper extremity, exercises for improving hand functions, stretching spastic muscles and medical treatment, and pulmonary rehabilitation program treatment. The patient did not have any secondary problem during his stay in our clinic. The last examination of the patient after his seven-month rehabilitation program in our clinic showed that his upper extremity muscle strength was 5/5, and bilateral hip flexors were 5/5, and bilateral knee flexors were 3/5, and bilateral feet dorsiflexors were 5/5, and extensor hallucis longus was 5/5 on the right and 4/5 on the left, and bilateral foot plantar flexors were 5/5. In the lower extremity, hip adductors had bilateral grade II spasticity, and hip flexors had grade II spasticity, and knee flexors had grade I spasticity, and Achilles tendon had bilateral grade II spasticity. Having been advised about requirements of his social life along with training about balance coordination, the patient was discharged with SPI ASIA D diagnosis. | ||||||
| ||||||
|
| ||||||
|
Discussion
| ||||||
|
We have presented this case in order to increase the awareness about being more careful against the risk of increased fractures in the spine of patients with AS when scheduling their fracture treatment in response to spinal injury resulting from trauma. Skull traction on 62- year-old patient with a 30-year history of AS diagnosis with isolated muscle strength loss following a traffic accident developed tetraplegia as a result of skull traction implementation after fracture. As the period of illness increases in patients with AS, compression-associated complications such as instability in spine, fractures, inflammation, posterior longitudinal ligament ossification, disc lesions and spinal stenosis might develop [4]. Clinical studies have shown that the risk of spinal cord injury is 11.4 times higher in patients with AS compared to the healthy population, and that fractures most frequently occur in cervical region despite the fact that they might occur in any part of the spine as well [5]. Cervical spine fracture is a serious life-threatening complication. The fracture might occur in any level of the spine, yet it is reported that it is particularly more frequent between cervical vertebrae [6]. The reason behind this is that osteoporosis which develops secondary to AS causes the spine to fail to absorb the energy of trauma leading to an intense buckling in the spine acting as a long lever arm [7]. Alaranta et al. reported that cervical spine injury in patients with ankylosing spondylitis is 17 times higher compared to the overall population [8]. The most widespread reason of SCI in patients with AS is falling. Patients with ankylosing spondylitis fall due to reasons such as deformation of their biomechanics, bad posture caused by vertebra loss, and displacement of balance center [9]. Another significant reason for SCI in patients with AS is traffic accident. Flexion injury in patients with AS causes fractures in vertebral bodies, while hyperextension injuries cause fractures penetrating into intervertebral discs [10]. Fractures in patients with AS occur, as the case with our subject, following hyperextension. Since spine elasticity is deformed in patients with AS, fractures such are burst fracture and compression fracture are rather rare [11]. Making a diagnosis based on direct radiographs in patients with AS, where minor trauma is present, might lead to wrong or delayed diagnosis due to the difficulty of visualizing lower cervical spinal cord and cervicothoracic junction, and due to the fact that ossified spinous ligaments deforms normal anatomy [12] [13]. CT and MRI scans are two of the appropriate diagnostic visualization options in patients with AS. Wrong choice of visualization method in diagnosis of fracture develop as a result of minor trauma in patients with AS doubles the risk of SCI [12]. Where there is suspicion of cervical injury in patients with AS, the neck must not be moved, and particularly collar and sand bags which force the neck to extension must not be used. Where there is suspicion of cervical fracture in patients with AS, first aid team should take measures ensuring positioning of the neck in slight flexion. Particular care must be exercised in visualization methods such as CT and MRI scans which forces the neck to hyperextension. As, extension positions might cause increase in neurological deficit [14]. As the case with our subject, implementing skull traction in these patients causes extension of vertebra applying a force on the vertebra similar to lever arm, leading to reduction of vertebral flexibility. This was a reason behind the patient's developing SCI similar to osteotomy in his cervical vertebra. Medical methods for treatment of vertebral fractures in patients with AS range from surgical fusion to protective halo use. A study comparing medical methods for vertebral fractures in patients with AS found no difference in terms of neurological and functional outcomes. Apple et al. reported in their study that hospital stay in patients who received non-surgical techniques for treatment of vertebral fractures was shorter. | ||||||
|
Conclusion
| ||||||
|
The way first aid team responds to patients with ankylosing spondylitis (AS) when they experience a trauma, and choice of radiological imaging, forcing to hyperextension during radiological visualization or factors which increase the load on bone, such as skull traction, during medical treatment increase neurological loss in these patients. The way to protect patients with AS against spinal cord injury is obtaining a detailed patient history, and requiring patients to wear medical tag, and creating awareness among first aid and radiology teams, and avoiding all practices which force these patients to hyperextension in any stage of medical intervention. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Emrullah Hayta – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Ahmet Karadağ – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Cesur Gumus – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2016 Emrullah Hayta et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|