|

|
 |
|
Case Report
| ||||||
| Massive recurrent fibrous histiocytoma of the frontonasal region: A case report | ||||||
| Fomete B1, Agbara R1, Adeola DS1, Idehen OK1 | ||||||
|
1Maxillofacial Unit, Ahmadu Bello University Teaching Hospital, Zaria, Nigeria.
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article: |
| Fomete B, Agbara R, Adeola DS, Idehen OK. Massive recurrent fibrous histiocytoma of the frontonasal region: A case report. International Journal of Case Reports and Images 2013;4(11):589–592. |
|
Abstract
|
|
Introduction:
Fibrous histiocytoma is the name for a group of lesions characterized by biphasic cell populations of fibroblast and histiocytes. Both benign and malignant forms have been described. The benign form often shows relapse following treatment and shows poor response to chemotherapy and radiotherapy. Therefore, radical excision or resection remains the therapeutic goal.
Case Report: Herein, we present a case of recurrent benign fibrous histiocytoma of the head and neck in a 25-year-old Nigerian male that was excised and skin grafted. Conclusion: Fibrous histiocytoma is less common in the head and neck region. | |
|
Keywords:
Fibrous histiocytoma, Recurrent, Frontonasal
| |
|
Introduction
| ||||||
|
Fibrous histiocytoma is a rare group of tumors with biphasic cell populations of fibroblast and histiocytes and which may exhibit benign or malignant features. Cutaneous and non-cutaneous forms have been described. Cutaneous fibrous histiocytoma refers to all superficial tumor of skin regardless of appearance while similar lesions involving the subcutaneous or deeper tissues are simply referred to as fibrous histiocytoma. [1] [2] In contrast to the malignant form, benign fibrous histiocytoma (BFH) of non-cutaneous tissues has received little attention in literature. [1] Less than 10 cases of non-cutaneous fibrous histiocytoma of the head and neck region have been reported in literature. [1] [2] [3] [4] Specific sites of involvement, on the head and neck region, described in literature, include buccal mucosa, submandibular triangle, tongue, larynx, nasal cavity, mandible and supraclavicular fossa. [4] We found no occurrence at the frontal region. Herein, we present a case of a 25-year-old Nigerian male with recurrent BFH, highlighting the challenges associated with oral surgical practice in a resource-poor environment. | ||||||
|
Case Report
| ||||||
|
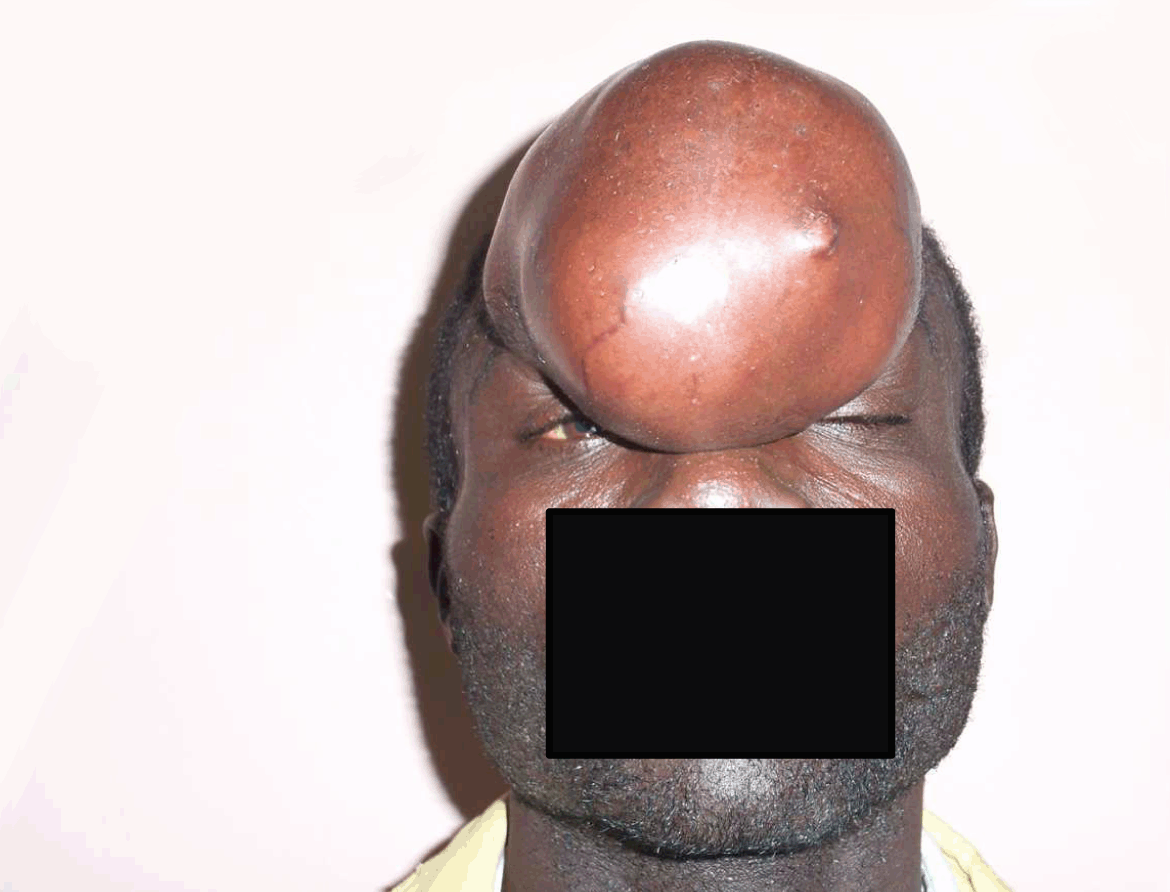
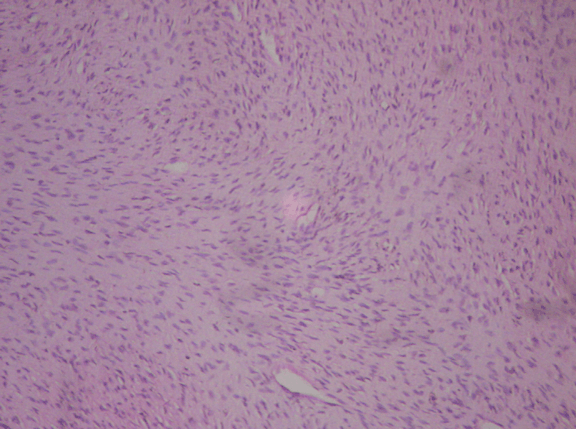
A 25-year-old male carpenter was referred to our clinic from the surgical outpatient department on account of recurrent frontonasal mass of two years duration. Swelling was first noticed 10 years ago following trauma to the frontal region and gradually increased in size. The excision of mass was done twice in a peripheral hospital and the last excision was two years prior to the presentation. The forehead was the initial site of involvement but swelling gradually expanded with each recurrence to involve the nasal region. Except for headache, all other medical history was not significant. Physical examination revealed a frontonasal mass involving both frontal regions but more to the right side, measures about 10 cm in its widest diameter, with some scares and some superficial vessels. (Figure 1) Surface was smooth but lobulated, firm in consistency and not tender. Swelling was attached to the underlying structures with involvement of the overlying skin. But the nasal cavity was free. Fine needle aspiration cytology (FNAC) revealed a benign lesion, voluntary retroviral screening was negative, full blood count and electrolyte, urea and creatinine were within normal range. Axial computed tomography (CT) scan revealed an extracranial mass of soft tissue origin with slight erosion of the frontal bone. The mass had a signal characteristics mimicking brain tissue. Patient had excision of mass under general anaesthesia with delayed split thickness skin grafting two months post excision to allow for adequate granulation tissue formation and possible recurrence. (Figure 2) He is currently on follow-up and doing well so far. Postoperative histology report grossly, a skin covered sessile polyp measuring 13.5x9x9 cm and weighs 434 g. Cut surfaces showed grey solid areas. Microscopy revealed a circumscribed dermal lesion lined by a focally atrophied, pigmented, keratinized epidermis. The lesion is composed of a mixture of plump spindle cells and histiocytes-like cells growing in a diffuse sheet. The stroma is abundant fibromyxoid to collagenized with foci of lymphocytic infiltrates and congested vascular channels. The deep margins appeared to be involved by the lesion. (Figure 3) | ||||||
| ||||||
| ||||||
| ||||||
|
Discussion
| ||||||
|
Benign fibrous histiocytoma was not recognized as a distinct clinical entity until the 1960s as a result of confusion regarding the natural history of fibrohistiocytic lesions. This confusion was settled following the development of immunohistochemical techniques and electronic microscopy. [1] [5] Benign fibrous histiocytoma occurs more in the upper and lower extremities and in the retroperitoneal region. Involvement of the head and neck region have been described and sites involved include buccal mucosa, submandibular triangle, tongue, larynx, nasal cavity, mandible and supraclavicular fossa. [1] This case is unique due to its site of presentation, the frontal region. The occurrence of fibrous histiocytoma has been associated with trauma, sun exposure and chronic infection. These have lead to the postulation that it represents a reactive proliferative lesion. [4] The patient in our case had a history of trauma to the frontal region following a fight, and noticed occurrence of initial mass one month later. The average duration of tumor occurrence in literatures ranges from 3–12 months. The BFH is seen commonly in young or middle age adults with a male predominance. The reported male to female ratio ranges from 1.9:1 to 2.5:1. [6] [7] The patient in our case was a 25-year-old male. Most patients presented to the hospital as a result of symptoms from interference with normal physiology of the involved area such as dyspnea, dysphagia, visual disturbance and headaches or present for esthetic reasons. [1] The patient in this case, reported a history of headache and was worried about his esthetics. The diagnosis of fibrous histiocytoma is made primarily from histologic examination of tissue samples in which conventional microscopy shows a mixed population of spindle shaped fibroblast and rounded histiocytes in varying proportions. [8] [9] The lesion in our case was composed of a mixture of plump spindle cells and histiocytes-like cells growing in a diffuse sheet. The stroma was abundant fibromyxoid to collagenized with foci of lymphocytic infiltrates and congested vascular channels. The maximum diameter has been reported to range from 2–12 cm. [4] In our case it was about 13.5 cm in its widest diameter. Electron microscopic and immunohistochemical studies though not specific, helps in differentiating BFH from aggressive fibrous histiocytic lesions such as malignant fibrous histiocytoma (MFH) and dermatofibrosarcoma protuberans. [10] With immunohistochemical studies, BFH shows a significant population of Xllla-positive cells with scanty CD4 positive cells. The reverse is the case with dermatofibrosarcoma protuberans. [10] [11] Other differentials to be considered are neurofibroma and leiomyosarcoma. Treatment in most cases is essentially local excision since it is neither radiosensitive or chemosensitive. There is no report of metastases, thus the prognosis is generally good. Recurrence has been reported and incomplete excision is believed to be a reason. [4] [12] About 12 out of 46 cases of benign fibrous histiocytoma followed-up, with a mean follow-up of three years, recurred. [6] The patient in our case report had two recurrences, the second recurrence occurring within one year of excision both in a peripheral hospital. In view of recurrent potential, patient should be promptly refer to the specialist and prolong follow-up, if not for life. | ||||||
|
Conclusion
| ||||||
|
Though less common in the head and neck region occurrence of benign fibrous histiocytoma may be associated with functional or aesthetic problems. Understanding its clinical behavior and histological features are vital in differentiating it from other lesions and in its management. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Fomete B – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Agbara R – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Adeola DS – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Idehen OK – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© Fomete B et al. 2013; This article is distributed the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any means provided the original authors and original publisher are properly credited. (Please see Copyright Policy for more information.) |
|
|